Gastroenterology
is concerned with diagnosing and treating conditions which affect the digestive tract. This can include conditions of specific organs within the system, but may also relate to secondary illnesses that indirectly affect digestion and the absorption of nutrients. Procedures for diagnosis and testing may include invasive techniques and surgery, but can also greatly rely upon imaging in order to determine the cause of the issue.
What Types of Illnesses Require Gastroenterology Procedures?
Problems with digestion and nutrient absorption can be mechanical or function based. This means that issues in one part of the digestive tract can be affecting overall health, but it also means that specific organ dysfunction or chronic illness may be impacting the symptoms that are expressed. For this reason, diagnostic procedures play a large part in determining the course of treatment. Some common issues that can require gastroenterological procedures include:
Any condition where digestion is adversely impacted can require a diagnostic procedure. Some imaging and exploratory techniques are also recommended as preventive care and may be performed during a regular physical. However, individuals who have specific concerns that relate back to the gastric function may be asked to undergo a number of tests in order to determine the cause of the problem.
What are Gastroenterology Procedures?
Many diagnostic and treatment techniques can be similar in gastroenterology, as they use imaging and exploration. However, surgery for treatment is not always necessary, and once the cause of the health problem has been uncovered, patients may be able to rely on medication to treat the illness. Some of the more common techniques which may be used for initial diagnosis and some forms of treatment include:
Colonoscopy
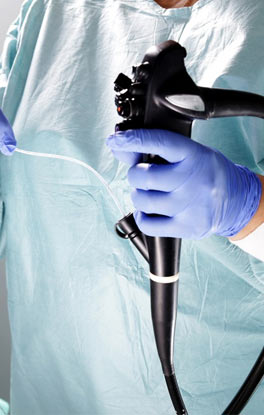
this procedure entails that a flexible camera is inserted through the rectum in order to view the lower colon. Although this is primarily an imaging technique, physicians may use the procedure to remove any polyps that are present. The technique is generally performed as an outpatient procedure, although patients may need a day for home recovery.
Endoscopic retrograde cholangiopancreatography (ERCP)
for this technique, a flexible camera is inserted down the throat, in order to view the esophagus, stomach, and upper part of the small intestine. This procedure also uses a contrast injection in order to view how the gall bladder is performing and determine at what point digestive function is disrupted. This is also an outpatient procedure, although the use of anesthesia requires some recovery time.
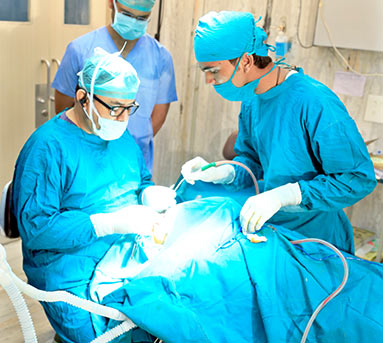
Laparoscopic surgery
although this is more common as a treatment technique, it is also used for diagnostic purposes. In these procedures, a small camera is inserted through a minimal incision in the abdomen for imaging purposes, while surgical tools are also inserted through this opening. Removal of polyps, parts of organs, and the appendix are all possible with this diagnostic and treatment technique.
Gastroenterology Treatments
Depending upon the nature of the impairment, most treatments for gastroenterological problems will either be through surgery or through medication. Surgical intervention will be most likely if there is the need for any of the following:
• Removal of diseases tissue – this can be the case if there are polyps or tumors present in the digestive tract or if there is infection in the tissues. In cases of appendicitis or Crohn’s disease, the removal of sections of the intestines can be common.
• Fecal diversion – compaction of fecal matter can occur through illness or through medication reactions. In these cases, surgery is required to remove the blockage or to change the path of the waste materials if parts of the intestines do not function.
• Internal stitching – in some cases, prolapsed may contribute to poor gastric function. If this is the problem, then surgery may be used to reattach prolapsed organs or parts of the intestine in order to promote proper physiological actions.
Surgery is not always required for the treatment of gastric illnesses, and in many cases, therapy can be a combination of lifestyle changes and medication. These may still be necessary even if surgery is needed, and will vary based on the condition that patients are managing. The use of nutritionists as well as specialized physicians can often allow for non-invasive alternatives to treatment.


